As Canada continues to grapple with a relentless stream of drug shortages, one in four adults in the country has either personally been affected in the last three years or knows someone who has, according to a survey commissioned by the Canadian Pharmacists Association.
“It’s really starting to become a much more dire situation in pharmacies,” said Phil Emberley, the association’s director of practice advancement and research, who also works as a pharmacist in Ottawa.
The problem has worsened over the last few years, Emberley said, to the point where the frequency of medication shortages is “unprecedented.”
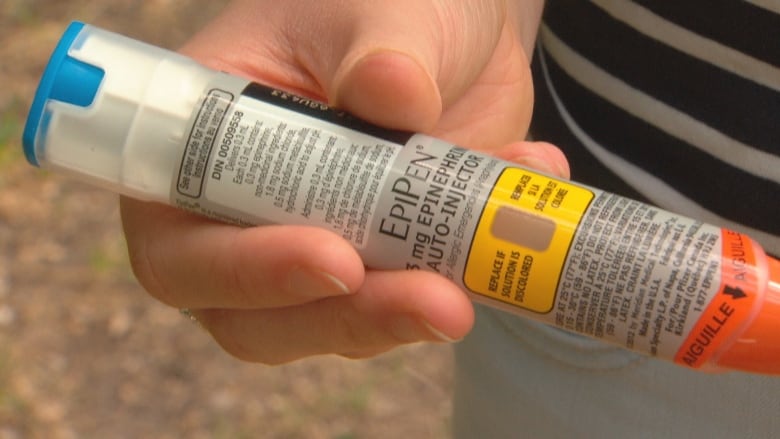
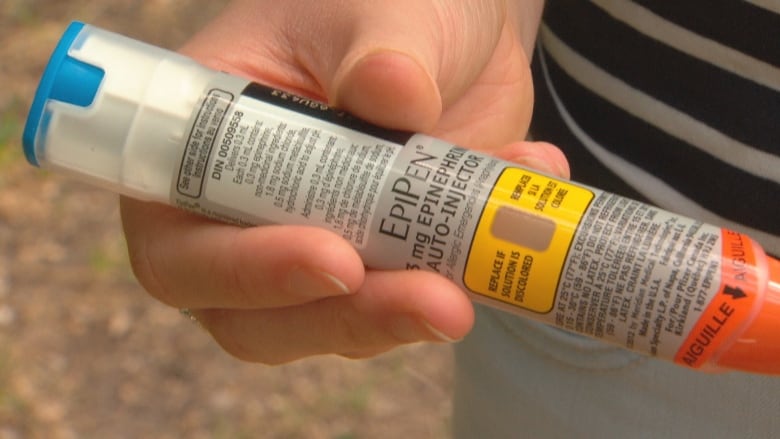
Last summer’s critical shortage of EpiPens, which many children with life-threatening allergies depend on to stop an anaphylactic reaction, drew public attention to the issue.
Then in November, the chronic drug shortage problem once again pierced people’s consciousness when pharmacies across Canada ran out of Wellbutrin, a widely used antidepressant. There are also recurring shortages of various blood pressure medications, including ARBs (angiotensin receptor blockers).
But these are just a few examples of a chronic problem. There are currently more than 1,690 medications listed in “actual shortage” status on Drug Shortages Canada, the federal government’s official tracking website.
EpiPen shortage
The EpiPen shortage was blamed on an issue with the autoinjector and the ARB shortage can likely be traced back to the recall of several medications containing valsartan, after batches manufactured at a Chinese plant were found to contain an impurity that is a suspected carcinogen.
But the root causes of drug shortages remain a mystery, although likely factors range from manufacturing issues to marketing and distribution decisions by pharmaceutical companies, experts say. Health Canada has repeatedly said it is aware of the drug shortage issue and working to find solutions.
When a medication runs out, doctors, nurse practitioners and pharmacists are usually able to deal with it by prescribing a similar drug, Emberley said. But in addition to the extra time and resources that extra work takes, it can also be stressful for patients — particularly those with chronic illnesses.
“A lot of people who are taking medication, they are responding to that medication in a positive way,” Emberley said. “So they’ve come to rely on the medication and when you say to them, ‘I’m really sorry but your medication is not available,’ they … become quite concerned.”
Switching medications as an ongoing response to shortages is also not good patient care, he said.
Alternative not always as effective
“The prescriber goes through … a very conscious decision to prescribe a certain medication and not another one,” he said. “The alternative may not be as effective.”
Dr. Iris Gorfinkel, a Toronto family physician, said the process of finding an alternative medication costs money — because patients whose prescriptions can’t be filled often have to return to their doctor’s office for yet another visit billed to the provincial health system.
“It resonates very deeply because as a family doctor it’s my job to make sure the patients get the drugs they need,” Gorfinkel said. “I have to kind of brainstorm with them to say, ‘OK what substitutions are there, if any, for the missing drugs.'”