Life expectancy: By 2030, many will live beyond 90 (research)
Life expectancy study shows many to live beyond 90 by 2030.
Average life expectancy is set to increase in many countries by...
Indian teenager wakes up headed to own funeral
Indian Teenager wakes up suddenly on his way to his own funeral.
An Indian teen has shocked doctors and his family after...
British Man Gets Pregnant: Hayden Cross Shows Baby Bump
British man gets Pregnant? Hayden Cross has put his gender transition on hold to have a baby after finding a sperm...
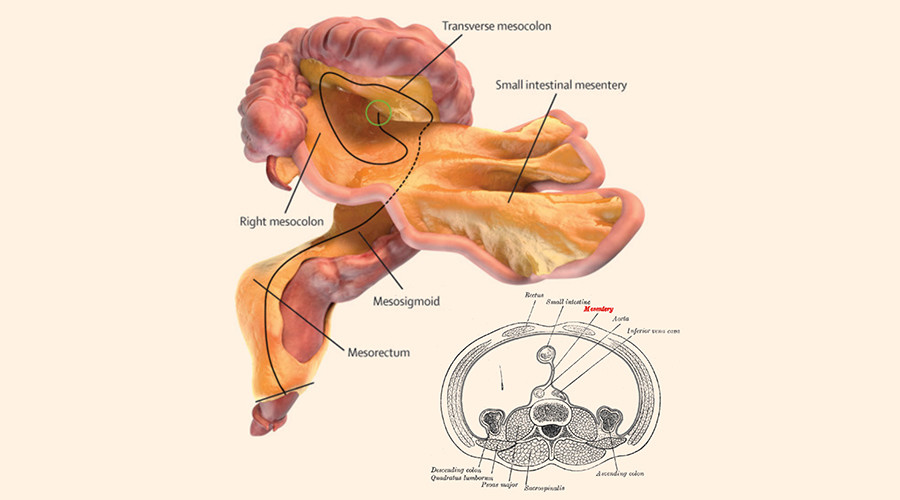
New human organ? Doctors discover new organ called mesentery in human body
A new human organ has been discovered hiding in the human digestive system.
A University of Limerick professor has identified an emerging...
Magic mushrooms eases anxiety in cancer patients, finds new research
Magic Mushrooms: Cancer Patients Could Find Relief in Psychedelic Drug.
Two studies published Thursday in the Journal of Psychopharmacology could open a...
Beth Goodier: ‘This Real Life Sleeping Beauty’ Has To Deal With Six-Month Naps
Beth Goodier, 22-Year-Old With "Sleeping Beauty Syndrome" Sleeps for Months at a Time.
On her 17th birthday, Beth Goodier fell asleep and...
Michael Funk: flesh-eating bacteria that killed man in four days expected to rise
Michael Funk was cleaning crab pots at his bayside condominium; four days later he was dead, the victim of flesh-eating bacteria.
Michael...
Boston: cat virus discovered in Mattapan
BOSTON —The Animal Rescue League of Boston has identified a potentially fatal virus outbreak affecting cats in Mattapan.
The disease in question...
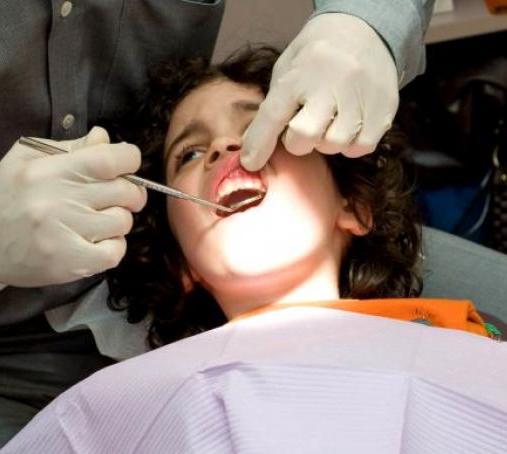
CDC: More low-income kids need dental sealants, Report
Dental sealants covering back teeth could prevent up to 80% of cavities in schoolchildren, according to a CDC Vital Signs report...
Separated Twins Continue Recovery [Video]
Conjoined twin brothers Anias and Jadon McDonald, who've been attached at the head for their entire 13 months of life, were...










![Separated Twins Continue Recovery [Video] Separated Twins Continue Recovery [Video]](https://webtopnews.com/wp-content/uploads/2016/10/Separated-Twins-Continue-Recovery-Video.jpg)