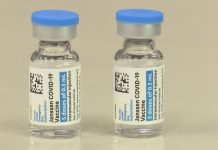
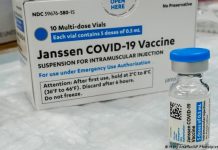
A BRAIN-SWELLING disease 75 times more deadly than Covid could mutate to become the next pandemic killing millions, scientists have warned.
Experts told Sun Online how a number of emerging diseases could trigger another global outbreak – and this time it could be ‘The Big One’.
The fruit bat-borne virus Nipah is a prime candidate for serious concern, they fear.
Severe brain swelling, seizures and vomiting are just some of the symptoms of this highly potent disease – which was first discovered in 1999 in Malaysia.
Outbreaks in south and south-east Asia show the virus to be extremely deadly, with a death rate of between 40 to 75%.
Covid-19’s fatality rate is around one per cent, according to Imperial College, so a Nipah pandemic would kill many more people.
It has also been named by the World Health Organisation (WHO) as one of 16 priority pathogens for research and development due to its potential to trigger an epidemic.
And chillingly, Nipah is just one of 260 known viruses with epidemic potential.
The virus is such concern due to its long incubation period of up to 45 days, meaning people could spread for over a month before falling ill, and its ability to cross between species.
Nipah also has an exceptional high rate of mutation and there fears a strain more well adapted to human infections could spread rapidly across the the well interconnected countries of South East Asia.
And while Covid-19 has devastated the world, killing almost 2.5million people, its already been warned the next pandemic could be much worse.
Dr Melanie Saville, director of vaccine research and development at CEPI, have warned The Sun Online the world needs to be prepared for the next “big one”.
The Sun Online previously scientists grave concerns over the threat of zoonotic diseases – when infections jump from animals to humans – and the danger of them causing a pandemic every five years.
Humans clashing with nature as populations expand and habitats get pushed back is considered to be a prime driver of new diseases – and that is exactly what happened with Nipah when it first infected pig farmers in Malaysia.
Dr Rebecca Dutch, chair of the University of Kentucky’s department of Molecular and Cellular Biochemistry and a world a leader in the study of viruses, told us that although there are no current Nipah outbreaks in the world, they occur periodically and it is “extremely likely” we will see more.
She told us: “Nipah is one of the viruses that could absolutely be the cause of a new pandemic. Several things about Nipah are very concerning.
“Many other viruses in that family (like measles) transmit well between people, so there is concern that a Nipah variant with increased transmission could arise.
“The mortality rate for this virus is between 45% and 75% depending on the outbreak – so this is much higher than Covid-19. Nipah has been shown to transmit through food, as well as via contact with human or animal excretions.
“The incubation period for Nipah can be quite long, and it can be unclear if transmission can occur during this time.”
As well as fruit bats, pigs have caught the disease by eating infected mangoes and have been known to pass the disease to humans.
More than one million pigs believed to be infected with the Nipah virus were slaughtered in Malaysia to prevent them from transferring it to humans.
Dr Jonathan Epstein, vice president for science and outreach at the EcoHealth Alliance, explained how they are tracking the Nipah virus and are worried about its potential.
He told us: “We know very little about the genetic variety of Nipah-related viruses in bats, and what we don’t want to happen is for a strain to emerge that is more transmissible among people.
“So far, Nipah is spread among close contact with an infected person, particularly someone with respiratory illness through droplets, and we generally don’t see large chains of transmission.
“However, given enough opportunity to spread from bats to people, and among people, a strain could emerge that is better adapted to spreading among people.
“This is a zoonotic virus knocking on the door, and we have to really work now to understand where human cases are occurring, and try to reduce opportunities for a spillover, so that it never gets the chance to adapt to humans.”